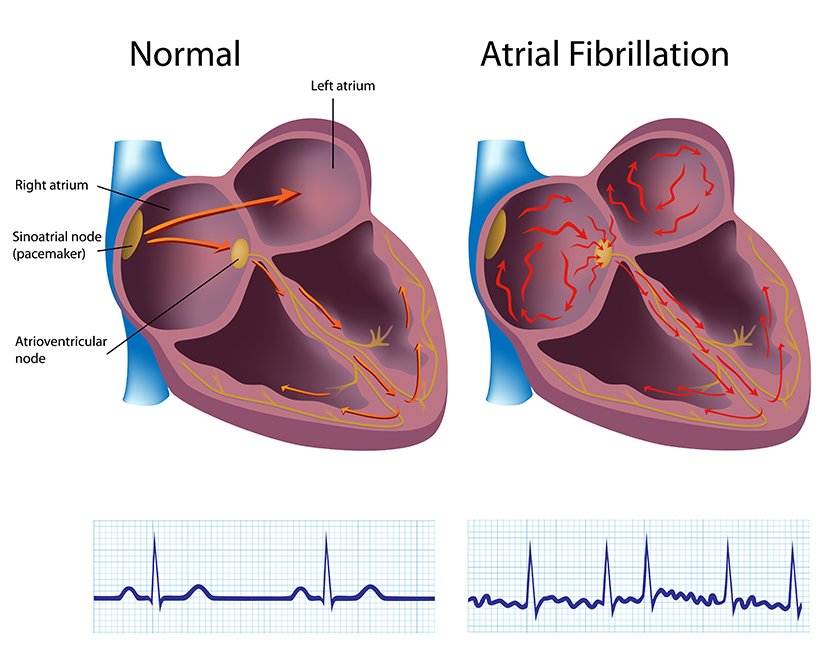
Longstanding persistent atrial fibrillation (LPAF) is an arrhythmia, or abnormal heart rhythm, that can cause serious complications if left untreated. Understanding the causes, symptoms, and treatments of LPAF is essential for anyone who suffers from this condition.
This blog post will cover the basics of what you need to know about LPAF and how it should be managed.
WHAT ARE THE CAUSES OF LPAF?
The exact cause of LPAF is unknown, but there are a few known risk factors that can increase your chances of developing this condition.
These include high blood pressure, diabetes, sleep apnea, coronary artery disease, thyroid disease, and an enlarged left atrium in the heart. Additionally, alcohol and drug abuse have been linked to an increased risk for LPAF.
SYMPTOMS OF LPAF
The most common symptom of LPAF is palpitations or a rapid heartbeat that may feel like your heart is skipping beats or racing uncontrollably.
Other symptoms can include:
- Shortness of breath,
- Dizziness or
- Lightheadedness,
- Chest pain or
- Tightness,
- Fatigue or weakness,
- Sweating.
If you experience any of these symptoms regularly or they become more severe over time it’s important to speak with your doctor so they can properly diagnose LPAF and provide appropriate treatments.
YOU MAY READ OUR OTHER BLOG TOO:
UNDERSTANDING AND TREATING PHLEBITIS AND THROMBOPHLEBITIS OF RIGHT FEMORAL VEIN
A BRIEF SUMMARIZATION Of BUDD-CHIARI SYNDROME
DIAGNOSIS OF SUBSEGMENTAL PULMONARY EMBOLISM
A BRIEF OVERVIEW OF LUPUS ANTICOAGULANT SYNDROME
COMPLICATIONS AND RISK FACTORS FROM LPAF
Longstanding persistent atrial fibrillation (LPAF) associated with several complications and risk factors, including:
- Stroke: LPAF increases the risk of stroke, as the irregular heart rhythm can cause blood clots to form in the heart, which can then travel to the brain and cause a stroke.
- Heart failure: LPAF can cause the heart to work harder, which can lead to heart failure over time.
- Heart valve damage: LPAF can cause damage to the heart valves, which can lead to leakage or stenosis.
- Age: LPAF is more common in older adults, with the risk increasing as people age.
- Hypertension: High blood pressure is a major risk factor for LPAF.
- Obesity: Obesity increases the risk of LPAF.
- Diabetes: People with diabetes are more likely to develop LPAF.
- Family history: LPAF is more common in people who have a family history of the condition.
- Alcohol consumption: Excessive alcohol consumption is a risk factor for LPAF.
- Sleep apnea : Sleep apnea is a risk factor for LPAF.
DIAGNOSIS AND TREATMENT
If you suspect you may have LPAF it’s important to speak with your doctor so they can perform tests such as an electrocardiogram (ECG) or echocardiogram (echo) in order to accurately diagnose the condition.
Once diagnosed there are several treatment options available including medications such as beta-blockers which help control your heart rate;
- Antiarrhythmic drugs which help regulate your heartbeat;
- Electrical cardioversion which delivers shockwaves directly into your heart in order to reset its rhythm;
- Catheter ablation which uses energy pulses delivered through catheters inserted into veins in order to destroy faulty electrical pathways;
- Surgical procedures such as Maze surgery which creates scar tissue in order disrupt faulty electrical signals causing AFib episodes.
- Additionally lifestyle modifications such as maintaining a healthy weight through diet and exercise can also help reduce AFib episodes in some people with this condition.
CONCLUSION
Longstanding persistent atrial fibrillation (LPAF) is a serious condition that requires proper diagnosis and treatment in order to reduce complications such as stroke caused by blood clots forming due to irregular heartbeat patterns. It’s important for anyone who suspects they may have this condition speak with their doctor so they can determine if further testing needs to be done and discuss potential treatments options available depending on their individual situation.
By understanding how this condition works it’s possible for those affected by LPAF to take steps towards managing their health better and reducing their risk for complications associated with this condition.
Patients who are on blood thinning medications such as WARFARIN [COUMADIN] are asked to monitor their PT/INR LEVEL on a regular basis. PATIENT SELF TESTING has made it convenient for people to easily perform their blood tests on their own with the help of PT/INR METERS at home and can get accurate reading in seconds.