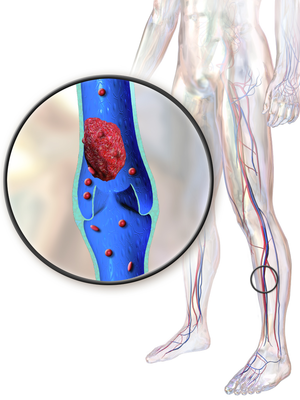
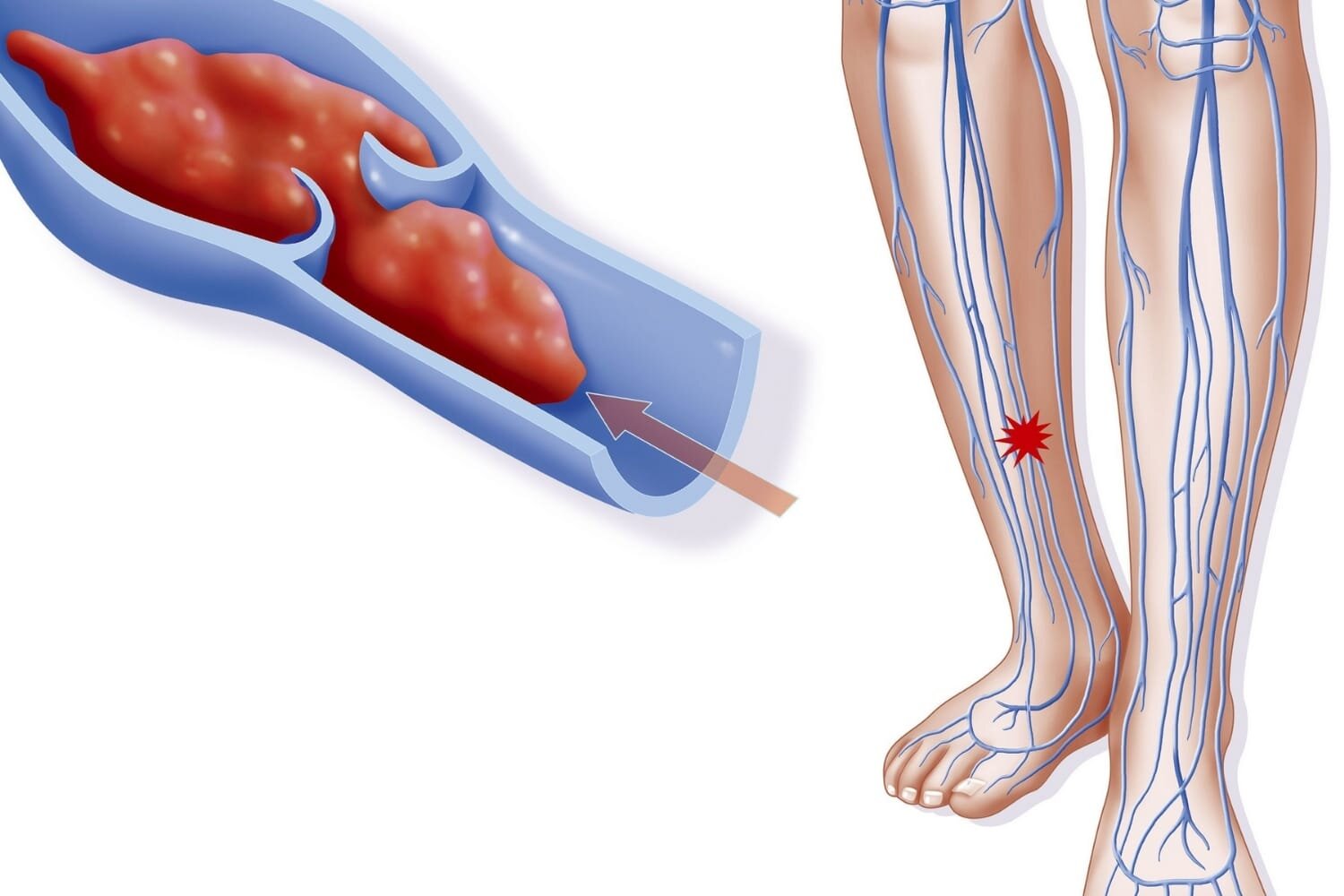
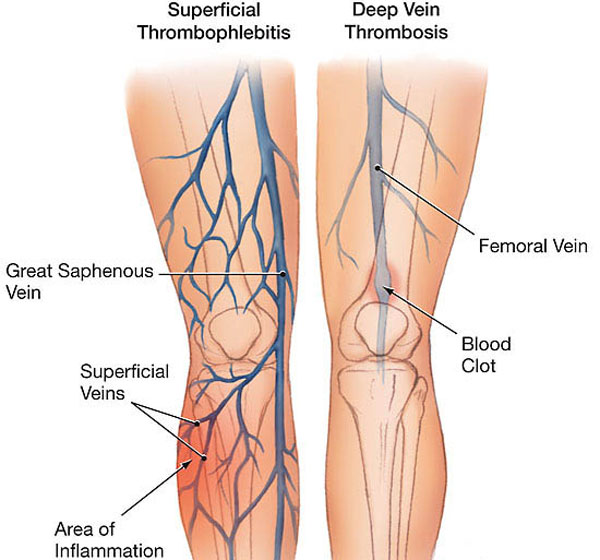
Phlebitis and thrombophlebitis are conditions that occur when a vein becomes inflamed and a blood clot forms. These conditions can occur anywhere in the body, but they are most common in the legs.
In this blog, we will be discussing phlebitis and thrombophlebitis of the right femoral vein.
CAUSES:
Prolonged sitting or standing: Sitting or standing for long periods of time can cause blood to pool in the legs, increasing the risk of blood clots and inflammation.
- Trauma to the vein: Trauma to a vein, such as a deep cut or bruise, can cause inflammation and increase the risk of a blood clot.
- Varicose veins: Varicose veins are abnormally enlarged veins that can cause blood to pool and increase the risk of blood clots.
- Blood clots: Blood clots can form in the veins, causing inflammation and increasing the risk of phlebitis and thrombophlebitis.
- Hormonal changes: Hormonal changes, such as those that occur during pregnancy or menopause, can increase the risk of phlebitis and thrombophlebitis.
- Certain medications: Medications, such as birth control pills, can increase the risk of phlebitis and thrombophlebitis.
- Cancer: Cancer and cancer treatments can increase the risk of phlebitis and thrombophlebitis.
- Obesity: Obesity increases the risk of phlebitis and thrombophlebitis as it causes extra pressure on the veins and makes it harder for blood to flow properly.
SYMPTOMS
The symptoms of phlebitis and thrombophlebitis can include:
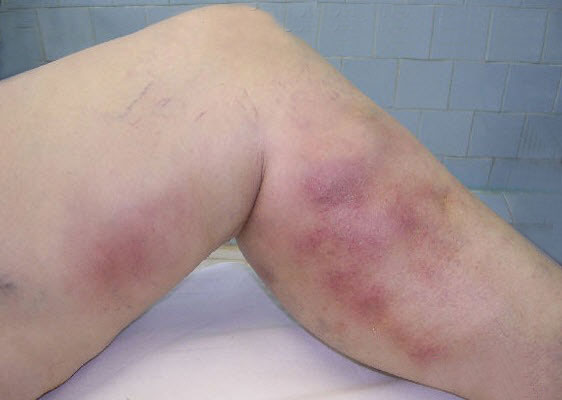
- Pain and tenderness in the affected area
- Swelling in the affected area
- Redness and warmth of the skin
- A palpable cord in the affected area
YOU MAY ALSO READ OUR OTHER BLOGS:
A BRIEF SUMMARIZATION Of BUDD-CHIARI SYNDROME
MULTIPLE SUBSEGMENTAL PULMONARY EMBOLI WITHOUT ACUTE COR PULMONALE
A SUMMARIZATION ON ACUTE EMBOLISM AND THROMBOSIS OF LEFT PERONEAL VEIN
COMPLICATIONS
If left untreated, phlebitis and thrombophlebitis can lead to serious complications, including:
- Pulmonary embolism
- Deep vein thrombosis
- Post-thrombotic syndrome
DIAGNOSIS
Phlebitis and thrombophlebitis can be diagnosed through a physical examination and imaging tests such as an ultrasound or CT scan. Your doctor may also order blood tests to check for clotting disorders.
LINE OF TREATMENT
- Compression stockings: These are special stockings that provide gentle pressure to the affected area, helping to reduce inflammation and swelling. They also help to improve blood flow and prevent the formation of new clots.
- Anti-inflammatory medication: Anti-inflammatory drugs can be used to reduce pain and inflammation associated with phlebitis and thrombophlebitis.
- Blood thinners such as WARFARIN: Blood thinners, also known as anticoagulants, help to prevent the formation of new clots and reduce the risk of complications. Warfarin is one of the most commonly used blood thinners for phlebitis and thrombophlebitis.
- Surgery to remove the clot: In some cases, surgery may be necessary to remove the clot and restore blood flow to the affected area. This is typically only done in severe cases where other treatments have not been effective.
It is important to note that treatment for phlebitis and thrombophlebitis will vary depending on the individual case and the underlying cause. Your doctor will work with you to develop a treatment plan that is best for you. It is also important to follow your doctor’s instructions and take all medications as prescribed.
Patients who are on blood thinning medications such as WARFARIN [COUMADIN] are asked to monitor their PT/INR LEVEL regularly. PATIENT SELF TESTING has made this very convenient as one can easily perform their blood tests on their own with the help of PT/INR METERS at home and can get the accurate readings in seconds